Bariatric Surgery
Bariatric surgical procedures cause weight loss by restricting the amount of food the stomach receives and intestinal malabsorption and more importantly by bringing neurohormonal changes in the body which causes less hunger and feeling of fullness and satisfaction.
Common Bariatric surgery procedures include Gastric Bypass, Vertical Sleeve Gastrectomy, Adjustable Gastric Band and Duodenal Switch.
Each surgery has its unique advantages.
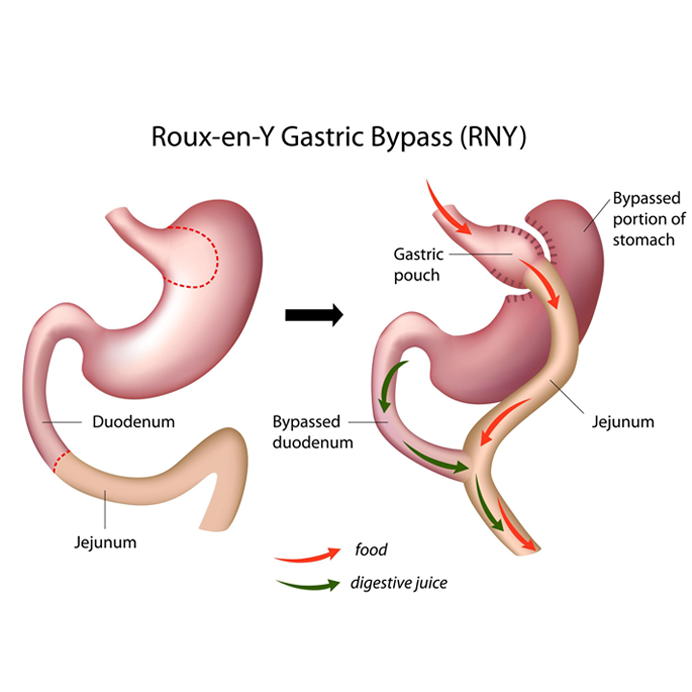
Gastric Bypass
The Roux-en-Y Gastric Bypass – often called gastric bypass – is considered the ‘Gold Standard’ of weight loss surgery. It is a 70 year old operation with excellent track record of safety and great outcomes.
The Procedure of Gastric Bypass
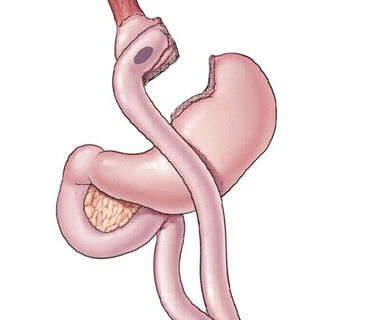
There are three components to the procedure. First, a small stomach pouch, approximately 30-45 milliliters in volume, is created by dividing the top of the stomach from the rest of the stomach. This forms the stomach pouch. This portion gives restriction. Next, the first portion of the small intestine is divided and this small intestine is brought up and connected to the above mentioned small stomach pouch. This part provides malabsorption and releases GLP-1 hormone.
The third aspect is to complete the joining of the other divided ends of small intestine. This way the excluded stomach and digestive enzymes from pancreas and liver are allowed to mix with food. This results in formal digestion of food and absorption of nutrients to sustain the body.
The rerouting of the food or “Bypassing” the normal digestive pathway is what produces changes in gut hormones that promote satiety, suppress hunger, and reverse one of the primary mechanisms by which obesity induces type 2 diabetes.
- Gastric bypass helps in significant long-term weight loss up to range of 60 to 80 percent of excess body weight.
- Also brings favourable neurohormonal changes in body and and restricts the amount of food that can be consumed.
- Resolution of Diabetes is up to 80%.
- High Blood Pressure is up to 70-80%.
- Sleep apnea is up to 80%.
- Resolution of Fatty Liver
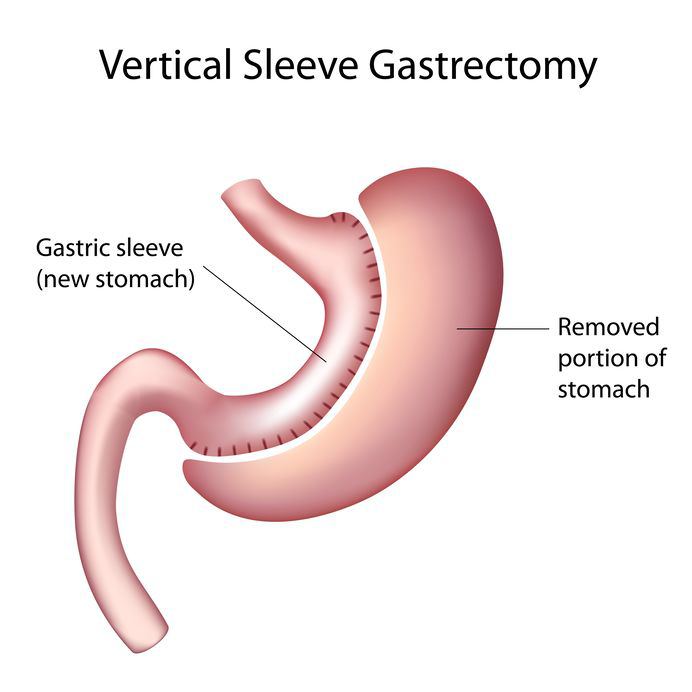
Sleeve Gastrectomy
The Vertical Sleeve Gastrectomy – often called the sleeve or just Sleeve gastrectomy – is performed by removing approximately 70- 80 percent of the stomach. The remaining stomach is a tubular that resembles a sleeve of the shirt or a banana.
The Procedure of Sleeve Gastrectomy
The key step in procedure of Vertical Sleeve Gastrectomy is removing the food storage portion of stomach called Fundus. This helps in early satiety, less hunger and feeling of fullness and satisfaction.
This is devices with the help of measuring devices called Bougies.
The new tubular stomach is small in volume and holds much smaller volume compared to a normal stomach. This helps is restricting the total calorie intake.
Also the hormone Ghrelin , which promotes hunger , is significantly reduced and this helps in suppressing hunger and is a big help.
Other favourable hormonal changes helps in control of blood sugar,
Vertical Sleeve gastrectomy (VSG) is a relatively new procedure compared to Gastric bypass. It has been around for 18-20 years.
Short term follow up studies have shown that VSG is an effective weight loss and antidiabetic surgery.
The complication rates of the sleeve fall between those of the adjustable gastric band and the roux-en-y gastric bypass.
- VSG helps in significant long-term weight loss up to range of 50-60% percent of excess body weight.
- Resolution of Diabetes
- Resolution of High Blood Pressure
- Resolution of Sleep Apnea
- Resolution of Fatty liver
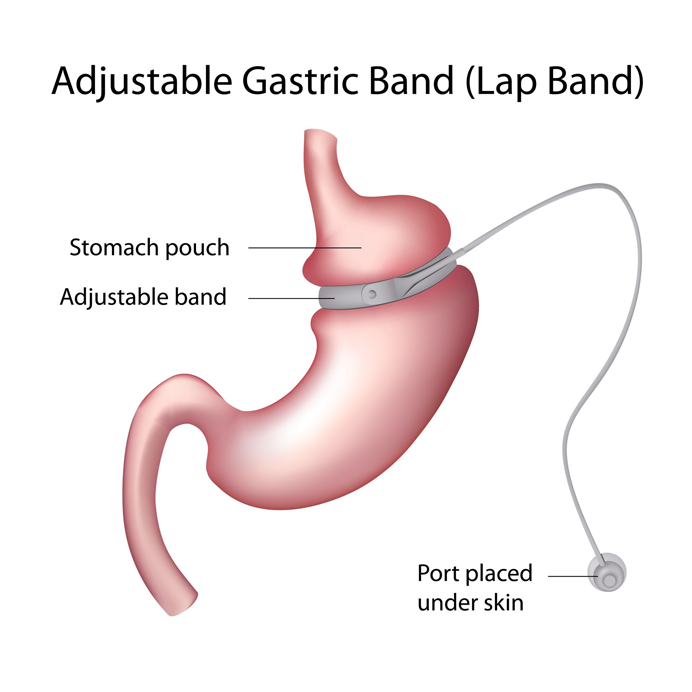
Adjustable Gastric Band
The Adjustable Gastric Band or just Band involves an inflatable silicone band that is placed around the upper portion of the stomach. This creates a small stomach pouch above the band. Rest of the stomach is below the band.
The Procedure of Adjustable Gastric Band
The Gastric Band works by creating a smaller stomach pouch. Eating small amount of food will satisfy hunger and gives feeling of fullness. The feeling of fullness depends upon the size of the opening between the pouch and the rest of the stomach, which is regulated by the gastric band. The band is adjusted by filling it with saline.
Reducing the size of the opening is done gradually over time with repeated adjustments or “fills.” This way band is a restrictive procedure and acts mainly by restricting the amount of food consumed by one.
There is no malabsorption. The clinical impact of the band seems to be that it reduces hunger, which helps the patients to decrease the amount of calories that are consumed.
- No Vitamin/ Mineral deficiency
- No Malabsorption
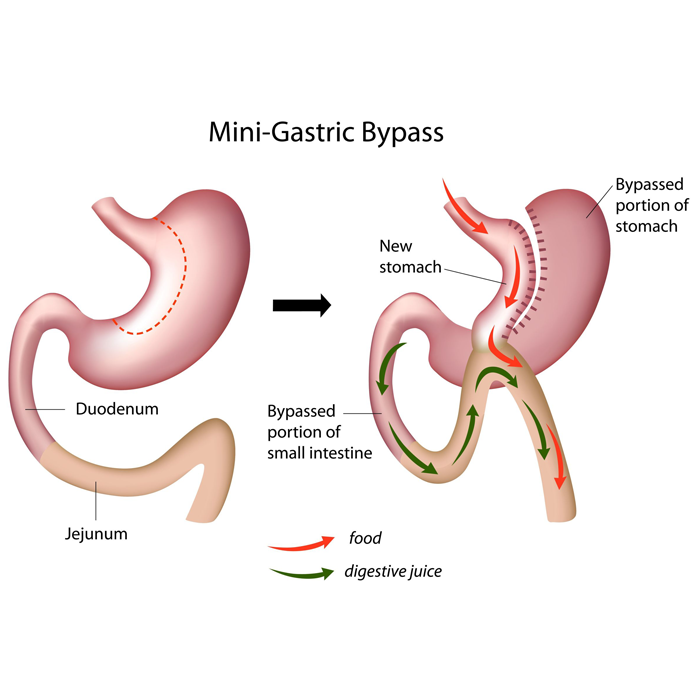
Biliopancreatic Diversion with Duodenal Switch (BPD/DS) Gastric Bypass
The Biliopancreatic Diversion with Duodenal Switch also known as BPD/DS – is combination of two procedures. First, a smaller, stomach pouch is created by removing a portion of the stomach, similar to the sleeve gastrectomy. Next, a large portion of the small intestine is bypassed.
The Procedure of (BPD/DS) Gastric Bypass
The duodenum, or the first portion of the small intestine, is divided just past the stomach. A segment of the distal (last portion) small intestine is then brought up and connected to the outlet of the newly created stomach, so that when the patient eats, the food goes through a newly created tubular stomach pouch and empties directly into the last segment of the small intestine. Roughly three-fourths of the small intestine is bypassed by the food stream.
The BPD/DS is considered to be the most effective surgery for the treatment of diabetes among those that are described here.
- Results in greater weight loss than RYGB, LSG, or AGB, i.e. 60 – 70% percent excess weight loss or greater, at 5 year follow up
- Allows patients to eventually eat near “normal” meals
- Reduces the absorption of fat by 70 percent or more
- Causes favorable changes in gut hormones to reduce appetite and improve satiety
- Is the most effective against diabetes compared to RYGB, LSG, and AGB